- HOME PAGE
- WELCOME TO BMA
- HIPAA AND PRIVACY PRACTICES
- "MYCHART" health portal
- MOUNT AUBURN HOSPITAL
- After Hours Emergency Calls
- PCP, NP and PA Profiles
- Our Specialists and Specialty Services
- MT AUBURN DIABETES CENTER
- ABOUT OUR OFFICE
- Being Our Patient
- REFERRALS : online request form
- Patient LIBRARY
- Turning 65? MEDICARE explained
- Medicare Annual Wellness Visit
- FIVE WISHES AND HEALTHCARE PROXY
- Social Work Care Coordination
- Quality Care Measures
- CareGroup Parmenter Home Care and Hospice
- MACIPA
- BULLETIN BOARD
- In Memoriam
- Job opportunities
BELMONT MEDICAL ASSOCIATES EARNS NATIONAL RECOGNITION FOR PATIENT-CENTERED CARE
NCQA Patient-Centered Medical Home™ standards emphasize enhanced care through
patient-clinician partnership
October 25, 2016, WASHINGTON, DC—The National Committee for Quality Assurance (NCQA) today announced that Belmont Medical Associates of Cambridge, MA has received NCQA Patient-Centered Medical Home (PCMH) Recognition for using evidence-based, patient-centered processes that focus on highly coordinated care and long‐term, participative relationships.
The NCQA Patient-Centered Medical Home is a model of primary care that combines teamwork and information technology to improve care, improve patients’ experience of care and reduce costs. Medical homes foster ongoing partnerships between patients and their personal clinicians, instead of approaching care as the sum of episodic office visits. Each patient’s care is overseen by clinician-led care teams that coordinate treatment across the health care system. Research shows that medical homes can lead to higher quality and lower costs, and can improve patient and provider reported experiences of care.
“NCQA Patient-Centered Medical Home Recognition raises the bar in defining high-quality care by emphasizing access, health information technology and coordinated care focused on patients,” said NCQA President Margaret E. O’Kane. “Recognition shows that Belmont Medical Associates has the tools, systems and resources to provide its patients with the right care, at the right time.”
To earn recognition, which is valid for three years, Belmont Medical Associates demonstrated the ability to meet the program’s key elements, embodying characteristics of the medical home. NCQA standards aligned with the joint principles of the Patient-Centered Medical Home established with the American College of Physicians, the American Academy of Family Physicians, the American Academy of Pediatrics and the American Osteopathic Association.
To find clinicians and their practices with NCQA PCMH Recognition, visit http://recognition.ncqa.org.
About NCQA
NCQA is a private, non-profit organization dedicated to improving health care quality. NCQA accredits and certifies a wide range of health care organizations. It also recognizes clinicians and practices in key areas of performance. NCQA’s Healthcare Effectiveness Data and Information Set (HEDIS®) is the most widely used performance measurement tool in health care. NCQA’s Web site (ncqa.org) contains information to help consumers, employers and others make more informed health care choices.
NCQA Patient-Centered Medical Home™ standards emphasize enhanced care through
patient-clinician partnership
October 25, 2016, WASHINGTON, DC—The National Committee for Quality Assurance (NCQA) today announced that Belmont Medical Associates of Cambridge, MA has received NCQA Patient-Centered Medical Home (PCMH) Recognition for using evidence-based, patient-centered processes that focus on highly coordinated care and long‐term, participative relationships.
The NCQA Patient-Centered Medical Home is a model of primary care that combines teamwork and information technology to improve care, improve patients’ experience of care and reduce costs. Medical homes foster ongoing partnerships between patients and their personal clinicians, instead of approaching care as the sum of episodic office visits. Each patient’s care is overseen by clinician-led care teams that coordinate treatment across the health care system. Research shows that medical homes can lead to higher quality and lower costs, and can improve patient and provider reported experiences of care.
“NCQA Patient-Centered Medical Home Recognition raises the bar in defining high-quality care by emphasizing access, health information technology and coordinated care focused on patients,” said NCQA President Margaret E. O’Kane. “Recognition shows that Belmont Medical Associates has the tools, systems and resources to provide its patients with the right care, at the right time.”
To earn recognition, which is valid for three years, Belmont Medical Associates demonstrated the ability to meet the program’s key elements, embodying characteristics of the medical home. NCQA standards aligned with the joint principles of the Patient-Centered Medical Home established with the American College of Physicians, the American Academy of Family Physicians, the American Academy of Pediatrics and the American Osteopathic Association.
To find clinicians and their practices with NCQA PCMH Recognition, visit http://recognition.ncqa.org.
About NCQA
NCQA is a private, non-profit organization dedicated to improving health care quality. NCQA accredits and certifies a wide range of health care organizations. It also recognizes clinicians and practices in key areas of performance. NCQA’s Healthcare Effectiveness Data and Information Set (HEDIS®) is the most widely used performance measurement tool in health care. NCQA’s Web site (ncqa.org) contains information to help consumers, employers and others make more informed health care choices.

The medical home is best described as a model or philosophy of primary care that is patient-centered, comprehensive, team-based, coordinated, accessible, and focused on quality and safety. It has become a widely accepted model for how primary care should be organized and delivered throughout the health care system, and is a philosophy of health care delivery that encourages providers and care teams to meet patients where they are, from the most simple to the most complex conditions. It is a place where patients are treated with respect, dignity, and compassion, and enable strong and trusting relationships with providers and staff. Above all, the medical home is not a final destination, instead it is a model for achieving primary care excellence so that care is received in the right place, at the right time, and in the manner that best suits a patient's needs.
Features of the Medical Home
The medical home is an approach to the delivery of primary care that is:
Features of the Medical Home
The medical home is an approach to the delivery of primary care that is:
- Patient-centered: A partnership among practitioners, patients, and their families ensures that decisions respect patients’ wants, needs, and preferences, and that patients have the education and support they need to make decisions and participate in their own care.
- Comprehensive: A team of health care providers is dedicated to the patient’s physical and mental health care needs, including prevention and wellness, acute care, and chronic care.
- Coordinated: Care is organized across all elements of the broader health care system, including specialty care, hospitals, home health care, community services and supports.
- Accessible: Patients are able to access services with shorter waiting times, "after hours" care, 24/7 electronic or telephone access, and strong communication through health IT innovations.
- Committed to quality and safety: Clinicians and staff enhance quality improvement through the use of health IT and other tools to ensure that patients and families make informed decisions about their health.
The following joint principles describe the characteristics of the
Patient Centered - Medical Home
Principles
Personal physician - each patient has an ongoing relationship with a personal physician trained to provide first contact, continuous and comprehensive care.
Physician directed medical practice – the personal physician leads a team of individuals at the practice level who collectively take responsibility for the ongoing care of patients.
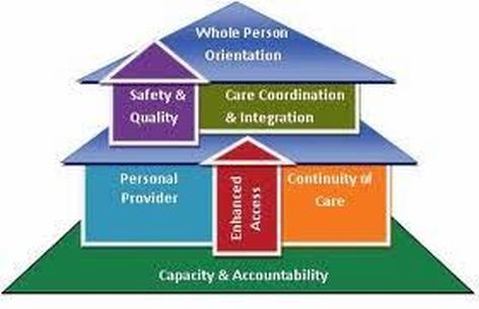
Whole person orientation – the personal physician is responsible for providing for all the patient’s health care needs or taking responsibility for appropriately arranging care with other qualified professionals. This includes care for all stages of life; acute care; chronic care; preventive services; and end of life care.
Care is coordinated and/or integrated across all elements of the complex health care system (e.g., subspecialty care, hospitals, home health agencies, nursing homes) and the patient’s community (e.g., family, public and private community-based services). Care is facilitated by registries, information technology, health information exchange and other means to assure that patients get the indicated care when and where they need and want it in a culturally and linguistically appropriate manner.
Quality and safety are hallmarks of the medical home:
Patient Centered - Medical Home
Principles
Personal physician - each patient has an ongoing relationship with a personal physician trained to provide first contact, continuous and comprehensive care.
Physician directed medical practice – the personal physician leads a team of individuals at the practice level who collectively take responsibility for the ongoing care of patients.
Whole person orientation – the personal physician is responsible for providing for all the patient’s health care needs or taking responsibility for appropriately arranging care with other qualified professionals. This includes care for all stages of life; acute care; chronic care; preventive services; and end of life care.
Care is coordinated and/or integrated across all elements of the complex health care system (e.g., subspecialty care, hospitals, home health agencies, nursing homes) and the patient’s community (e.g., family, public and private community-based services). Care is facilitated by registries, information technology, health information exchange and other means to assure that patients get the indicated care when and where they need and want it in a culturally and linguistically appropriate manner.
Quality and safety are hallmarks of the medical home:
- Practices advocate for their patients to support the attainment of optimal, patient-centered outcomes that are defined by a care planning process driven by a compassionate, robust partnership between physicians, patients, and the patient’s family.
- Evidence-based medicine and clinical decision-support tools guide decision making
- Physicians in the practice accept accountability for continuous quality improvement through voluntary engagement in performance measurement and improvement.
- Patients actively participate in decision-making and feedback is sought to ensure patients’ expectations are being met
- Information technology is utilized appropriately to support optimal patient care, performance measurement, patient education, and enhanced communication
- Practices go through a voluntary recognition process by an appropriate non-governmental entity to demonstrate that they have the capabilities to provide patient centered services consistent with the medical home model.
- Patients and families participate in quality improvement activities at the practice level.